Thanks to a pioneering research project at the University of Gothenburg, a group of women have gained new uteri through transplantation. In September 2014, the first child was born to a woman with a transplanted uterus: a healthy boy whose development was entirely normal. This has been followed by several births, first in Sweden and more recently in other counties as well, after knowledge transfer from the team at the University of Gothenburg.
After more than a decade’s preparations and collaboration between the multidisciplinary transplant team and members of the Ethical Forum at Sahlgrenska University Hospital, and several national, regional and local conferences regarding the project had been held. Thereafter, in May 2012, the team was authorized by the Regional Ethical Review Board in Gothenburg to carry out up to ten uterine transplants. This authorization included the proviso that the project must be subject to supervision by an independent safety committee.
Transplant in April 2013
The first transplant, on 15 September 2012, was followed by eight more in 2012 and 2013. In most cases the donors were the recipients’ mothers; in others, they were other close relatives or friends.
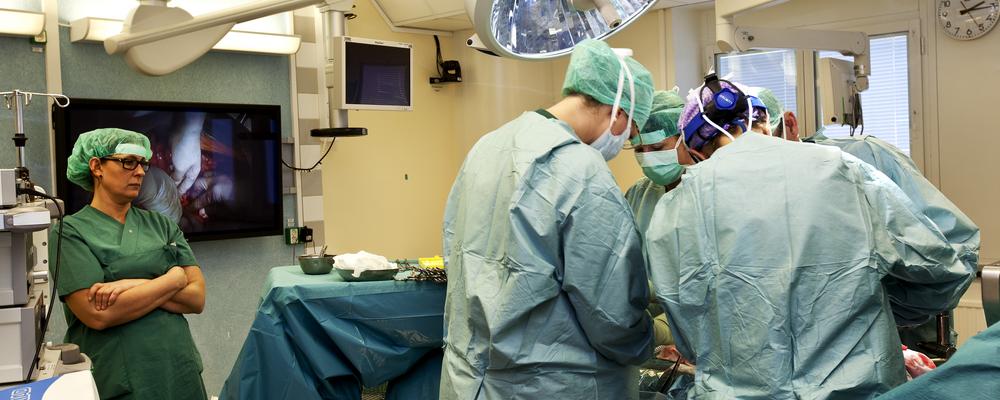
The operations were performed on weekends at Sahlgrenska University Hospital, in a surgical unit normally closed. Postoperative care of the women was provided by voluntary extra staff, and research funding from a private foundation covered all costs of staff and medical care. The transplants thus caused no disruption of normal care services.
Gynaecologists, anesthesiologists and transplant surgeons made up the team that operated on the donors and recipients. Surgeons from the U.S., Spain and Australia also took part. Using animal models, the team had practised the procedure together for several years.
Refinement of surgical technique
In the course of the transplantations, their logistic efficiency has steadily improved. The duration of the donor surgery has been reduced from 13 to 10 hours, which may be regarded as reasonable for this type of operation.
To date, the transplanted uterus has been removed in two of the nine women. In one case this was because of blood clots in the transplanted blood vessels. In the other, a uterine infection prompted the removal. In the other seven women, menstruation restarted roughly two months after the transplant. This outcome is judged to be a very good result.
IVF treatment
All the transplant patients were examined twice a week during the first month after the operation; once a week over the next two months; and every second week after that. In several cases, mild rejection reactions were found and treated successfully with medication. After six months, it was possible to reduce the immunosuppressive agent to a relatively low dose in a majority of patients.
A year after the transplants, attempts to achieve pregnancy began. This was done by placing embryos, conceived through IVF (in vitro fertilization) before the transplantation, in the transplanted uterus.
First birth
By spring 2014 the first pregnancy had started, and in September of the same year, one of the recipient women gave birth to a healthy, well-developed boy. This was the first baby in the world to be born from a transplanted uterus. Since then, another seven children have been born within the framework of this initial research project. These eight are the first children worldwide to have been born following uterine transplantation.
Modified technique
In May 2017 the first uterine transplant took place in what the researchers call the “robot project.” The new technique — robot-assisted keyhole surgery — represents a major technical advance and, for the donors, considerably less invasive procedures. The number of transplants in this project, too, is capped at ten.
Transplantation in November 2018
During surgery on the donor, the robot arms work through three incisions one centimetre long. The robot’s camera, inserted into a fourth incision, can be placed very close to the point where the surgery is underway, and also provides the surgeon with a highly magnified image. This technique, therefore, enables surgeons to perform the procedure with extreme precision. A hand movement from the surgeon can be converted into a millimetre-sized movement in the donor’s abdomen, allowing accuracy that minimizes disturbance to both the patient and her uterus.
The operating environment is also completely different. Two of the surgeons sit with their heads close to their respective covered monitors, on which they get an excellent three-dimensional view. They use joystick-like tools to steer the robot arms and surgical instruments that release the uterus. The operation ends with the removal of the uterus through an incision in the abdomen and its immediate insertion into the recipient by means of traditional open surgery.
Robot-assisted keyhole surgery has reduced blood losses and brought about shorter hospital stays. It means that donors feel better after the procedure.
Future prospects
The uterine transplant trials in Gothenburg are the world’s first systematic, research-based studies aimed at finding a treatment for women affected by uterine infertility. The project includes monitoring of several parameters of a medical and psychological nature and related to the quality of life, over several years. This will greatly benefit the further development of this type of transplantation. Currently, it is not clear when and how these transplants can become accessible to a larger group of patients.